Navigating the Realities of Cervical Vertigo
Cervical vertigo is a type of vertigo that is caused by a problem in the neck, specifically the cervical spine. The cervical spine consists of the seven vertebrae that make up the neck region of the spine. When there is a problem with the cervical spine, it can cause a range of symptoms including dizziness and vertigo.
Vertigo is the sensation that the environment around you is spinning or moving when it is still. People who experience cervical vertigo often describe a feeling of unsteadiness or dizziness when they move their head or neck. They may also feel a sense of imbalance or disorientation when they are standing or walking.
It can be caused by a variety of factors, including degenerative changes in the cervical spine, neck injuries, and inflammation of the joints in the neck. The condition can also be associated with other cervical spine conditions such as cervical spondylosis, cervical stenosis, and cervical disc disease.
It can be challenging to diagnose as the symptoms are like those of other vestibular disorders, such as benign paroxysmal positional vertigo (BPPV), but with the help of a neurotologist, patients can receive the care they need to manage their symptoms and improve their quality of life.
A neurotologist will perform a thorough evaluation of the patient’s symptoms and medical history, as well as a physical examination, to rule out other potential causes of vertigo.
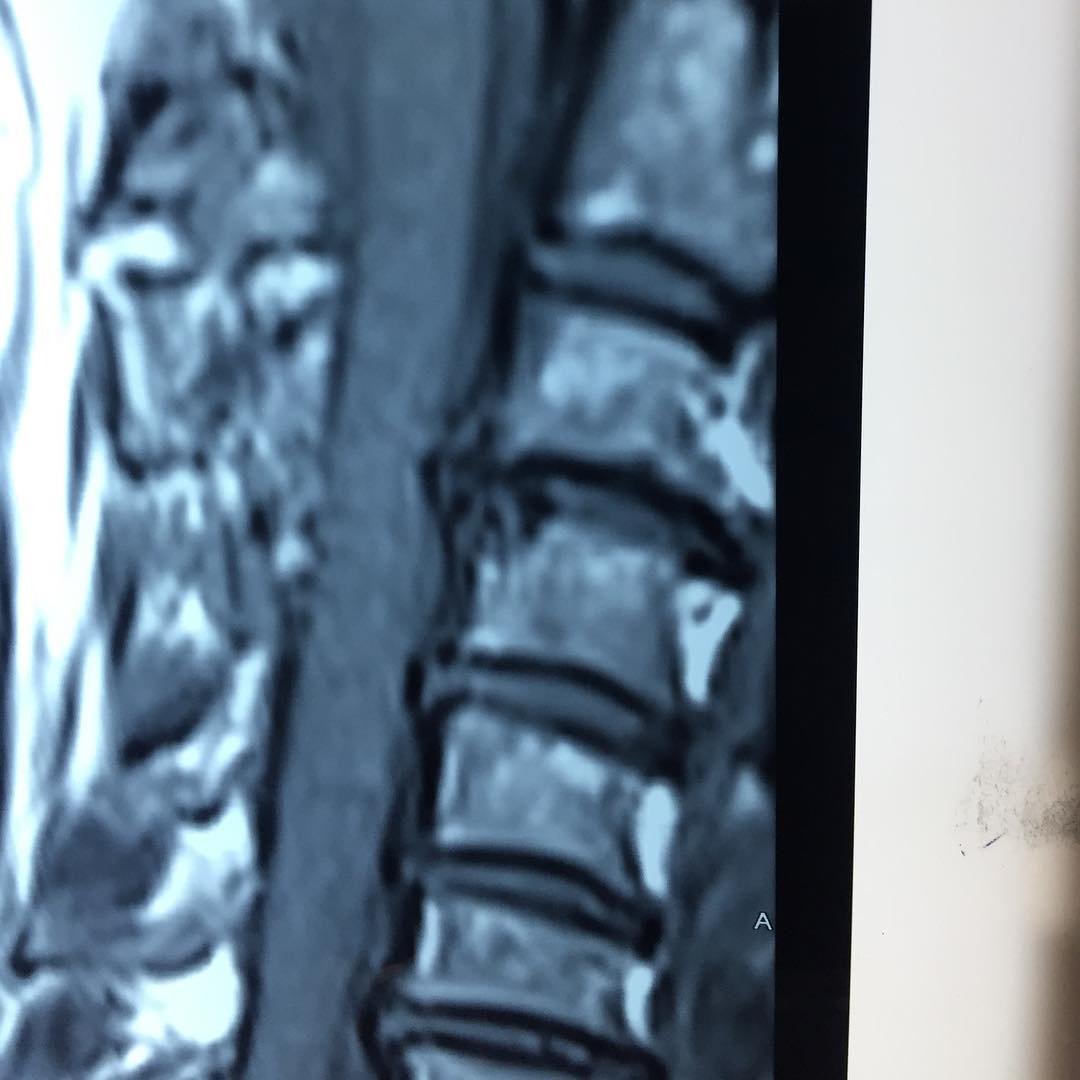
Imaging tests such as X-rays, MRI or CT scans may be ordered to assess the cervical spine for any structural abnormalities or changes.
Treatment for cervical vertigo may involve a combination of medication and physical therapy. Medications such as muscle relaxants and anti-inflammatory drugs can help to reduce pain and inflammation in the neck. Physical therapy may involve exercises to improve range of motion and strengthen the muscles of the neck and shoulders.